In the late 2000s, researchers working in villages along the border of Thailand and Cambodia discovered that circulating strains of Plasmodium falciparum, the parasite responsible for most malaria deaths, were evolving resistance to artemisinin-based drugs. Artemisinin-based drugs are the primary means of treating this deadly disease, which accounts for an estimated 227 million illness episodes and 627,000 deaths every year globally, with the heaviest burden among young children in sub-Saharan Africa.
Widespread drug resistance would be devastating to the global fight against malaria if effective alternatives were not found. The World Health Organization thus began coordinating efforts to contain the spread of these resistant parasites beginning in 2013. Yet resistance continued to appear across the region, leading to a shift in strategy in 2015: the countries of the Mekong sub-region agreed to an audacious goal of eliminating P. falciparum altogether by 2025 and all forms of malaria by 2030.
At the request of ministries of health and with financial support from the Bill & Melinda Gates Foundation, CHAI began providing support to governmental malaria programs in the region in 2015 to assist them in reorienting activities aiming to control the disease burden towards those that would eliminate it. Disease elimination requires comprehensive surveillance systems to understand where transmission is happening and what root causes are enabling it to continue. It requires ensuring access to high-quality diagnosis and treatment services for all who are sick with malaria, and the implementation of context-appropriate interventions to kill or prevent malaria-transmitting mosquitoes from biting a person.
Due in part to CHAI’s support, progress achieved by the countries of the region since 2015 has been historic. Malaria cases have plunged across the Mekong countries – Thailand, Myanmar, Laos, Cambodia, and Vietnam – from about 330,000 in 2015 to under 80,000 in 2021. In the Eastern Mekong countries of Cambodia, Laos, and Vietnam, where CHAI has embedded staff at both national and sub-national levels to help central and provincial government staff accelerate progress, reported malaria cases have fallen from approximately 130,000 in 2015 to fewer than 9,000 in 2021, a 93 percent decrease.
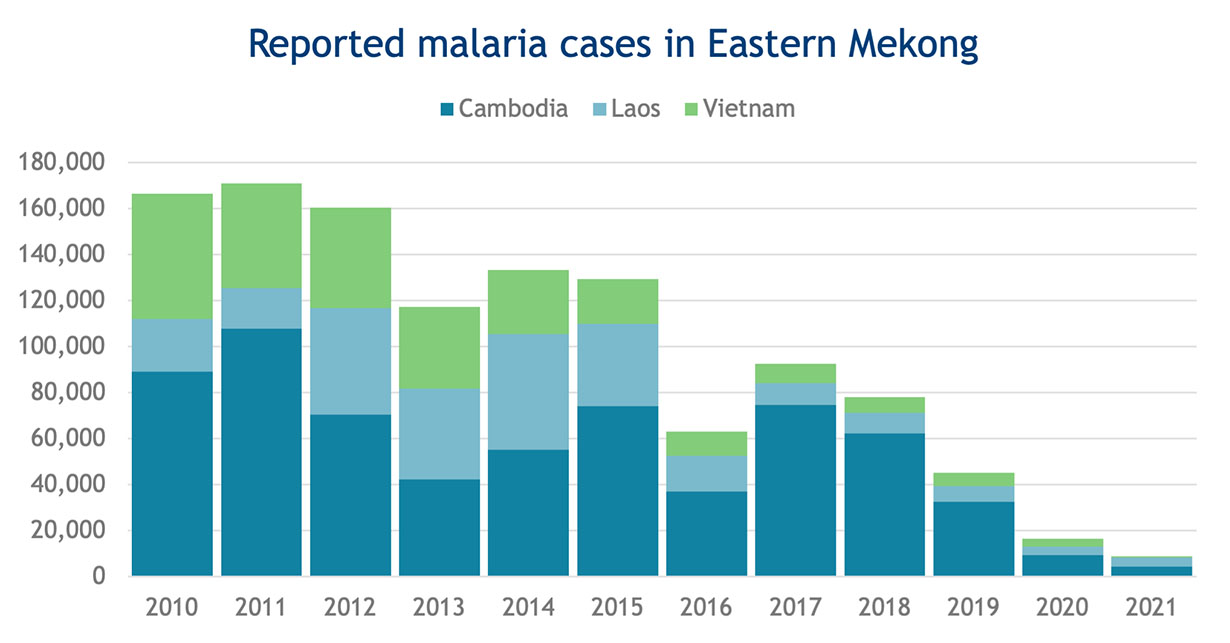
Cambodia, Laos, and Vietnam have achieved these gains through advances in data-driven programming. All three countries have invested heavily in improving information systems to allow high-resolution data on where malaria cases occur, what coverage is being achieved with preventative tools such as malaria bed nets, and whether sufficient access to case management services is being maintained throughout the region. In Laos for example, CHAI helped integrate digital systems for monitoring test and drugs stockouts with health information systems so that a sufficient supply of necessary commodities can be managed proactively. In Vietnam, CHAI assisted with replacing the paper-based surveillance system with an electronic one to allow fast, accurate reporting from across the country.
Quality disease surveillance allows programs to ensure effective tools and treatment are available and actively used in the places where they can be most impactful. In Cambodia, for example, CHAI helped the program reconstitute and expand a community health worker network that had ceased to function in 2015. Because community health workers live and work in affected communities, they can be a valuable source of timely care for sick patients. By 2020, the revigorated network was responsible for identifying over 60 percent of the malaria cases observed in the country.
The final push to elimination in these countries will not be without its challenges. Now that case counts are so low, there is a risk of donors losing enthusiasm for continuing to fund anti-malaria efforts and potentially pulling their funding before the sustainable endpoint of a malaria-free region is achieved. Governments must also keep up efforts even as malaria becomes less of a visible threat. Doing so will require innovation, such as potentially expanding the roles of community workers to treat other diseases to ensure they continue being useful sources for malaria care for the populations they serve.
Malaria elimination in the Mekong region can be achieved in the next few years. This accomplishment will be historic, but the fight against drug resistance will continue in the region and elsewhere. Recently, initial signs of parasite resistance to artemisinin-based drugs have been observed in several parts of sub-Saharan Africa. Can the Mekong’s success be echoed in the world’s highest endemic countries? It will be a tremendous challenge, but this World Malaria Day, success in the Mekong should give us reason for hope.






