Digital reporting tool and package of supportive interventions have improved malaria reporting and quality of care in the private sector.
BACKGROUND
Uganda has made significant progress over the past decade in reducing its malaria burden. Prevalence has decreased from 42% in 2009 to just below 10% in 2019. Despite this progress, Uganda has the 3rd highest global malaria burden (5%) and the 7th highest level of malaria-attributable deaths (3%).
In Uganda, more than half of febrile children one of the first symptoms of malaria, first seek treatment in the private health sector which is largely made up of clinics, pharmacies and drug shops. Yet, these private providers do not report into any national surveillance system, limiting our understanding of where malaria cases occur or what kind of treatment patients receive.
APPROACH
One of the strategic objectives of the Uganda Malaria Reduction and Elimination Strategic Plan (2021-2025) is to enhance the quality of malaria services in the private sector so that at least 80% of private facilities are managing malaria according to national guidelines and reporting quality data by 2025 (i.e., patients receive a confirmatory diagnosis and an ACT when positive). To help the National Malaria Control Division (NMCD) achieve its objectives, CHAI piloted a mobile reporting tool, called mTrac, in 136 private drug shops and clinics in four high-burden districts (Apac, Kole, Kwania, and Oyam), starting in 2019, to help strengthen surveillance and reporting into the national Health Management Information System.
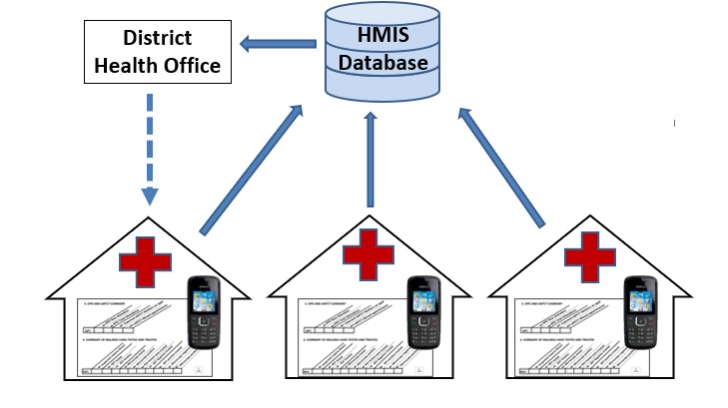
Figure 1: mTrac data flowchart
Although centered around the rollout of mTrac, the implementation included supporting interventions, such as case management and stock management trainings, targeted monthly supportive supervision visits by district health teams, support to form drug shop associations (DSAs) and data review meetings at the district-level.
IMPACT
Overall, the package of interventions including training, on-site mentorship, supportive supervision, and introduction of the mTrac tool to private providers showed improvements in provider knowledge, practices, and reporting for malaria, pneumonia, and diarrhea. There was a significant increase in the number of shops submitting weekly reports for malaria, pneumonia and diarrhea (21% at baseline and 90% at endline) [OR:41, p<0.01]. As a result of improved surveillance, increased private sector cases and testing data were captured into the national surveillance system.
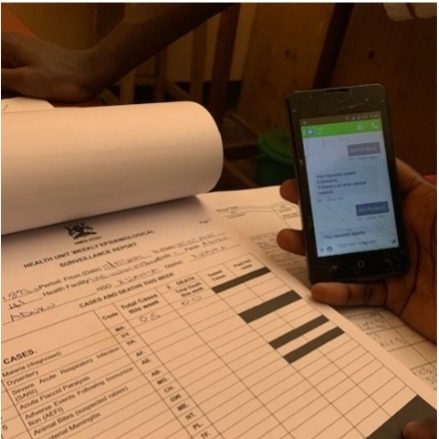

Figure 2: Shop attendant demonstrating how to use app during supportive supervision visit in Kole district
MOVING FORWARD
Based on the pilot, the NMCD is scaling mTrac and private sector case management to 54 additional districts. CHAI continues to provide technical assistance to the NMCD and implementing partners of the scale-up based on the lessons learned and experience from the pilot. Key lessons learned from the study included:
- Private providers will report weekly when using a simple digital tool that requires few indicators. Supporting providers with reminders to report helps to maintain engagement.
- Knowledge and practices for malaria, pneumonia and diarrhea can be improved in private health facilities with training, mentorship, and routine supervision.
- As a result of improving surveillance, capturing private sector cases and malaria tests has improved in DHIS2.
- Involvement of district health teams is key to ensuring sustainability and buy-in
- Grouping private health care providers into DSAs enhances easy coordination and activity implementation.
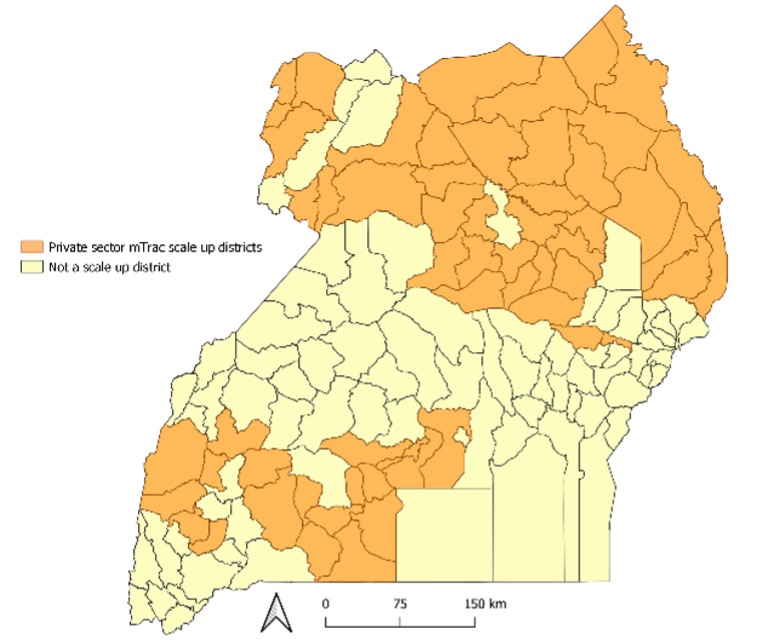
Figure 3: mTrac scale-up districts
Estimates suggest national scale-up could help capture an additional ~117K malaria cases/month which otherwise would be missed. A comprehensive surveillance system with private sector data will provide the NMCD with a more accurate picture of malaria burden and help inform where to target interventions including bed net campaigns.






