Living in a small town in the southern part of Ghana, Frema delivered her last two healthy babies at the nearby regional hospital. On her third delivery at the same facility Adiza, the midwife, informed her about the need to screen the baby for sickle cell disease (SCD), an inherited blood disorder. Babies with SCD are more vulnerable to bacterial infection and other life-threatening conditions.
Frema was anxious–this was the first time such a test was being requested for an otherwise healthy baby. Azida explained the disease, symptoms, and impact on the overall quality of life SCD could have on the child. Frema consented to having Kwadwo, her baby, screened.
Kwadwo tested positive for SCD. Frema found it hard to receive the news. She was worried about raising a child with sickle cell disease, as her two other children were frequently ill, often because of respiratory infections. When Adiza heard this, she was concerned and asked Frema questions about the health of her two other children.
“The symptoms Frema told me pointed me more towards sickle cell disease than any other disease,” said Adiza. Her aunties had told her it is an asthmatic trait in the family that cannot be treated at the hospital, and Frema received all sorts of mixtures to be given to the children any time they were unwell. This is what happens, and we end up losing the children at the last minute on the wards. I had to try and convince her to bring the other two children in to be seen by the pediatrician.
Frema did bring her two- and four-year-old back to the hospital and after additional tests, both were diagnosed with sickle cell disease. Frema received counseling on SCD, the symptoms her children may experience, and how to identify early warning signs that indicate the children need to be seen by a healthcare provider and how to care for them should they experience pain crises. Her children were enrolled at the facility’s pediatric sickle cell clinic. They have been on treatment since and are much healthier.
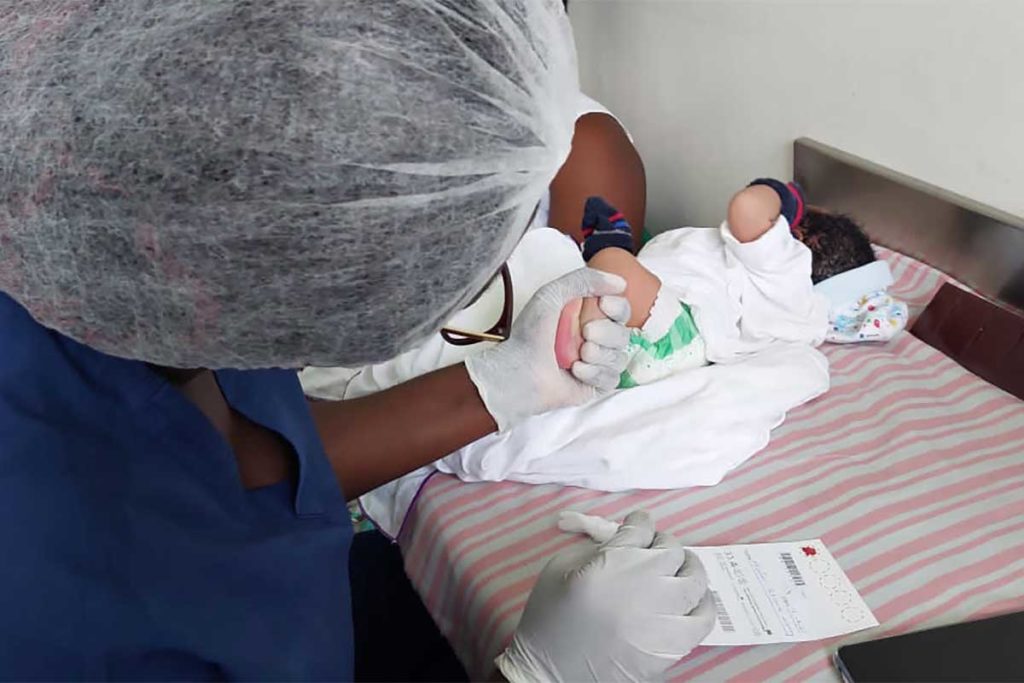
A trained nurse taking sample from a newborn using the heel prick method.
What is sickle cell disease?
An estimated 25 percent of Ghanaians carry the sickle cell trait,[1] with two percent of infants likely to be born with sickle cell disease each year.[2] SCD is an umbrella term for a group of inherited disorders where a gene mutation causes red blood cells to have an abnormal crescent shape [3]. These cells are rigid, blocking smaller blood vessels and preventing oxygen from reaching parts of the body[4]. This can lead to debilitating pain and other complications.
Without proper diagnosis and access to simple preventive treatment, 50 to 90 percent of newborns with sickle cell anemia, the most severe form of the disease, risk dying before their fifth birthday.[5][6] Yet, most infants remain undiagnosed and do not have access to treatment.
Closing the loop
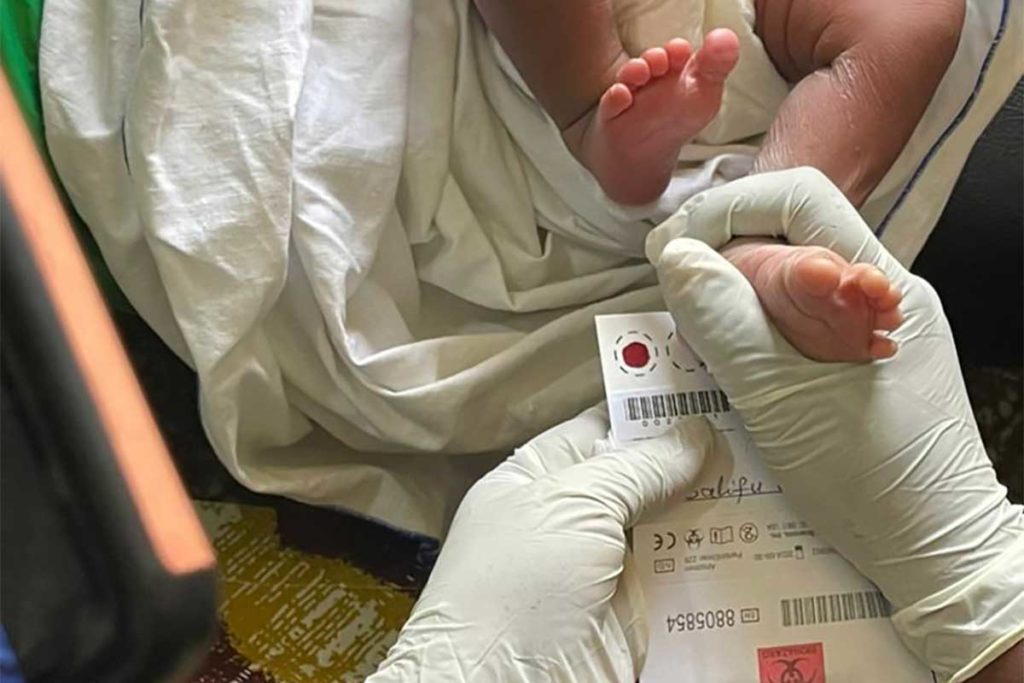
A master trainer demonstrates how to collect a dry blood spot sample needed for sickle cell disease screening.
Previously, sickle cell screening was only available in two regions within Ghana, meaning most newborns in the country did not have access to screening services.
In early 2021, CHAI, in collaboration with the Ghana Health Service and the Sickle Cell Foundation of Ghana, began working to close the loop between diagnosis and treatment of the disease. We began supporting the training of over 35 health workers in six hospitals to conduct newborn screening for sickle cell disease in their respective hospitals. In October, the second phase of training for 45 healthcare workers in an additional seven hospitals, across new regions, took place. In parallel, CHAI helped bring implementing partners and national stakeholders together to create a steering committee to guide the scale-up of the newborn screening program. Our goal–that trained health workers would become master trainers who would share their skills with colleagues in their facilities, while the stewardship of the steering committee would help bring together all partners working on sickle cell disease in Ghana.
Today, 11 out of 16 regions of the country offer newborn screening for sickle cell disease. The additional sites have already screened over 3,000 babies in the last three months. Once infants have been diagnosed, they are linked to specialized care and treatment, which for many includes penicillin to minimize the risk of dangerous infections. In addition, health workers provide caregivers with post-diagnosis counseling.
By February 2022, 20,000 newborns who would otherwise not have access to this service will have been screened. With more trained health workers and facilities providing SCD screening and treatment, we can diagnose more infants early for mothers like Frema, improve the quality of life of their children and reduce preventable deaths.
The Bill and Melinda Gates Foundation supports this work.
For more information, please contact Leslie Emegbuonye at lemegbuonye@clintonhealthaccess.org and Enyo Nudo at enudo@clintonhealthaccess.org.
[1] STTI, B. and Ohene-Frempong, K., 2008. Healthcare provision for sickle cell disease in Ghana: challenges for the African context. Diversity in Health and Social Care, 5, pp.241-54.
[2] Therrell Jr, Bradford L., et al. “Empowering newborn screening programs in African countries through establishment of an international collaborative effort.” Journal of community genetics 11.3 (2020): 253.
[3] Kato, G., Piel, F., Reid, C. et al. Sickle cell disease. Nat Rev Dis Primers 4, 18010 (2018). https://doi.org/10.1038/nrdp.2018.10
[4] Sickle Cell Disease, World Health Organization, Regional Office for Africa. https://www.afro.who.int/health-topics/sickle-cell-disease
[5] World Health Organization. Be smart, Know about Sickle Cell Disease! 2018. https://www.afro.who.int/news/be-smart-know-about-sickle-cell-disease.
[6] World Health Organization. Be smart, Know about Sickle Cell Disease! 2018. https://www.afro.who.int/news/be-smart-know-about-sickle-cell-disease.





