On November 12, 2015, 78 private sector healthcare providers attended trainings held in Dar es Salaam, Tanzania on malaria rapid diagnostics tests (mRDT). From September-November of this year, participants from health facilities in eight regions in Tanzania were invited to two-day training sessions. Two providers, including clinicians and lab technicians, from 593 facilities, representing nearly 60% of Tanzania’s formal private sector facilities, were invited in the hopes of educating at least one provider per facility on the proper use of mDRTs.
Historically, Tanzania has experienced a high prevalence of malaria, though statistics have improved drastically in recent years. In 2007, the national average malaria prevalence was roughly 18%, while only 9.5% four years later in 2011. The National Malaria Control Program (NMCP) has developed a national strategic plan through 2020 to reach even more ambitious goals of reducing the country’s malaria burden. To help achieve these goals, the NMCP’s current guidelines state that all suspected malaria cases should be confirmed parasitologically using either mDRTs or microscopy in an effort to improve malaria case management and reduce the wastage of subsidized Artemisinin Combination-Based Therapy (ACT) drugs.
Since 40% of Tanzanians seek care for fever in the private sector, it is essential that these facilities are equipped to provide malaria diagnosis. While Tanzania’s public sector has had access to mRDTs and proper training on usage since 2011, the private sector has had access to mRDTs but little formal training. Therefore, many private sector providers have not used mRDTs to diagnose even when available and instead treat patients presumptively without confirmatory testing. Others provide mRDTs, but with gaps in quality due to lack of training.

This training aims to fill this gap by providing healthcare workers with the necessary knowledge to diagnose and treat suspected malaria cases and educating them about the current malaria statistics in the country. By the end of the course, participants will be able to correctly use mRDTs and interpret the results, follow updated diagnosis and treatment guidelines for both uncomplicated and severe malaria, and report mRDT data into Tanzania’s Health Management Information System.
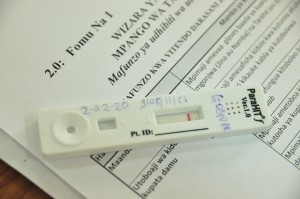
In today’s morning session, participants practiced performing the 15 steps of administering the mRDT on one another, critiqued by peers and supervised by trainers. Participants carefully checked product expiration dates, swabbed fingertips, drew blood samples to drop onto the test, and patiently waited for the timers they set to reach 20 minutes to read and record the developed test result. After the practice tests, participants discussed and read results together.
A training participant, Fahima Salim Suleiman, found the course helpful, including the instruction on properly administering the test. “Especially”, she said, “the time it takes—20 minutes—to read the mRDT and other areas where mistakes occur.”
Jancan Nakame, a participant currently working at a dispensary in Dar es Salaam, learned about the advantages of mDRTs opposed to other lab-based testing methods, such as microscopy.
“Because [mRDTs] take a shorter time, I can increase the number of tests performed per day because they could cover a lot of people, especially in this area of Dar es Salaam,” he said.
CHAI is supporting the NMCP to achieve Tanzania’s strategic goal of reaching 80% of suspected malaria patients with confirmatory diagnosis to improve malaria case management and reduce unnecessary ACT usage by millions of treatments. In the formal private sector, CHAI is working in close collaboration with NMCP and PSI to support the nationwide mRDT trainings, specifically by redesigning the training curricula to be more dynamic and focused on provider trust in the mRDTs and providing logistical and coordination support. NMCP oversaw the trainings, with PSI also providing significant technical support, as well as funding for the 2015 trainings through UNITAID.
In 2016, this training will be expanded to the remainder of the country’s formal private sector facilities. To further advance CHAI’s goal of scaling up diagnosis through mRDTs across the private sector, CHAI is also working closely with NMCP to advocate for and implement the scale up of a national policy change to allow the informal private sector, including private drug shops and pharmacies where many rural patients access malaria treatment, to perform mRDTs.