In Mathare Valley, one of Nairobi’s oldest and more impoverished slums, residents are crowded, and many lack access to basic services such as clean running water, electricity, and sanitation. As a result, the population suffers not only from extreme poverty, but also from a number of serious health ailments. Children are particularly susceptible; common pediatric ailments include dysentery, malnutrition, tetanus, tuberculosis, and skin and eye infections, among others.
However, despite the challenging conditions, dedicated health workers are committed to improving the health of Mathare’s population. CHAI is proud to support their efforts through drug and commodity procurement work, and integrated training and educational programs that help these healthcare workers diagnose and treat the slum’s most vulnerable residents: young children.
The Huruma Lions Health Center in Mathare Valley, Nairobi is an epicenter for health care in the area, serving the Mathare and Huruma slums. The facility’s catchment population is over 125,000; as a result volumes are high and the center is constantly busy. On a day in mid-March, the sounds of babies crying, mothers soothing, and children running and playing carried throughout the ward. Many of those waiting to be seen were there to access care for dehydration and diarrhea, which are particularly rampant in the slum, as a result of poor sanitation and unclean conditions.

Diarrhea is the second leading killer of children worldwide, responsible for nearly 600,000 deaths each year. In Kenya alone, an estimated 19,000 children under the age of 5 die annually as a result of diarrhea. If left unmanaged, diarrhea can progress to severe dehydration which in turn leads to shock and eventually death.
CHAI, with support from IKEA Foundation, is working to manage child diarrhea and reduce resultant child mortality in Kenya through a strategy that addresses knowledge, perception, and commodity gaps. Often, mothers, caregivers, and healthcare workers do not know enough about the signs and symptoms of diarrhea and dehydration in order to identify it as a problem. If they do, many do not perceive diarrhea to be life-threatening and thus do not seek care when appropriate, or until it is too late. Lastly, many facilities, pharmacies, and retail outlets lack the high-quality recommended treatment commodities to properly treat children at risk for severe diarrhea and death. Therefore, CHAI’s objectives for helping the Ministry of Health (MOH) manage child diarrhea in Kenya seek to address these gaps, based on source of care.
At the level of the home, for mothers and caregivers who do not seek care in a health facility, CHAI has worked with the MOH and other partners to encourage care-seeking behavior using multi-language mass messaging efforts to increase awareness and has partnered with key opinion leaders in communities to spread the word.
At the facility level, CHAI’s work includes the programming and implementation of Integrated Management of Childhood Illness (IMCI) training among health workers in both the public and private sectors, enabling workers to conduct a comprehensive needs assessment of a child, thereby not missing diarrhea or other pressing health issues and effectively and holistically treating the patient. Work also includes commodity management support to prevent stockouts of essential products and ensure the best treatment is affordable and available to children, and scale up of integrated health talks in which diarrhea is highlighted and discussed to change perception. Thus far, approximately 3,000 healthcare workers have so far been trained in IMCI.
The culmination of this strategy to prevent and treat child diarrhea in Kenya are the oral rehydration therapy (ORT) corners in health facilities throughout the country. ORT corners serve as accessible emergency centers for rehydration, referral, and education. Dehydrated children identified during the triage process are immediately brought to the ORT corners where they are given the first dose of ORS solution, a formula that replaces fluids and essential salts lost to dehydration, as well as zinc and Vitamin A. Caregivers are educated on preventative measures as well as the appropriate treatment and recommended feeding. ORT corners have also been implemented in pediatric wards to serve children admitted with severe dehydration. CHAI has supported the introduction of ORT corners in 448 health facilities by supplying IMCI-trained healthcare workers with ORT kits that include water storage, infection control methods, and ORS mixing equipment.
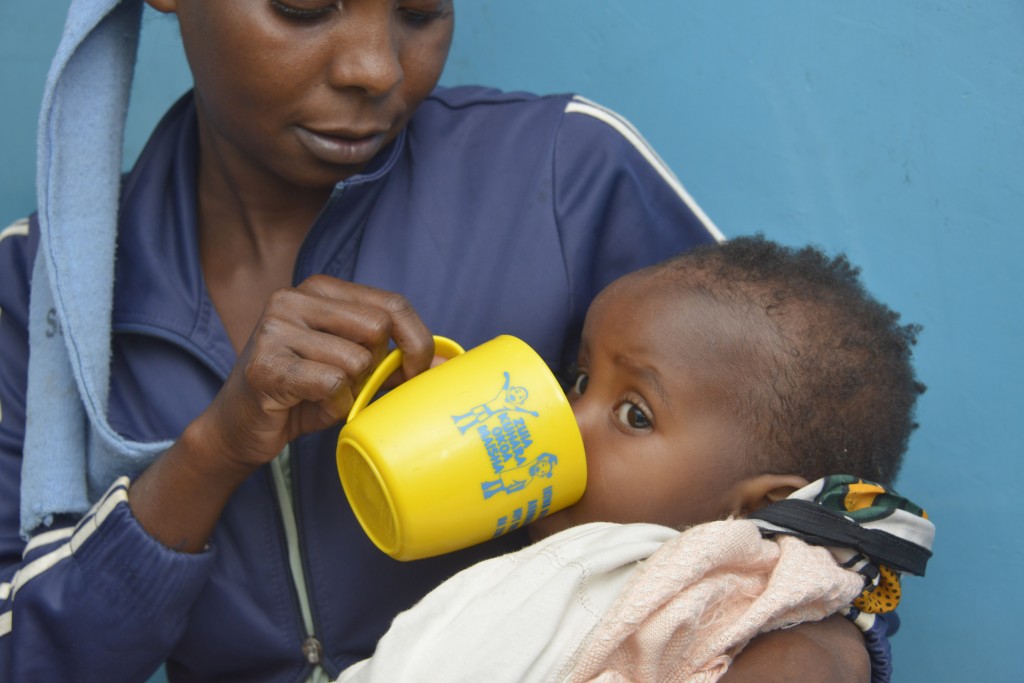
At Huruma Lions Health Center on a day in March, community health volunteer Tabitha Kanini was busy in the ORT corner with a listless dehydrated young girl suffering from diarrhea and her mother. Tabitha—who works as an unpaid volunteer—boiled water to sanitize it before showing the mother proper hand washing techniques, and filled an empty clean glass soda bottle to display proper measurement ratios for mixing the ORS sachet with water before giving the orange mixture to the little girl, whose blank eyes and clinginess showed her lack of energy due to dehydration.

Tabitha’s calm and patient demeanor when administering counseling and treatment and her solid knowledge of proper treatment practices were effective; after quietly gulping a few cups of the ORS mixture, the child began to look around the room with curiosity for the first time since coming in. She would be seen by a clinician as a follow-up to ensure she was no longer dehydrated before continuing treatment at home under the care of her mother. It is the dedication of community health volunteers like Tabitha and her manager, the facility nurse-in-charge Elizabeth Tsuna—both of whom have undergone CHAI-supported IMCI training—that make Huruma Lions Health Center a standout facility despite the area’s glaring challenges.


Elizabeth and rest of the health center’s staff are sticklers for data collection, monitoring, and evaluation, as evidenced by the large-scale charts and tables posted all over the facility. In her office, Elizabeth displays a facility workload monitoring table that keeps track of patient visits in 26 priority areas including diarrhea in children under 5, sexually transmitted infections, malnutrition, epilepsy, family planning, and full immunizations at the health center. In the ORT corner, she displays a detailed chart outlining diarrhea/dehydration-specific monthly statistics and progress since January 2014. She shows us that since the IMCI training and provision of CHAI-provided ORT corner supplies—including not only zinc and ORS used to treat diarrhea, but also water containers, cups, measuring jugs, and posters with diarrhea prevention and treatment messages —incidence of severe dehydration has decreased significantly at the facility. Thus far in 2015 there had been no cases of severe dehydration. It is her goal that no child progress to that stage this year. As a result of her and her staff’s hard work, the Nairobi City Council awarded Huruma Lions Health Center as the city’s best performing health center.


Through productive partnership led by the MOH, county health management teams, CHAI, and other partners, the uptake of ORS, zinc and the combined zinc/ORS therapy in Kenya has increased. ORS uptake increased from 39 percent in 2009 to 64.5 percent in 2014. Similarly, more children with diarrhea received zinc at 8.1 percent compared to 0.2 percent in 2009. The proportion of children receiving the combined therapy has also increased to 7.5 percent from 0.2 percent in 2009. Despite the amazing work of Tabitha, Elizabeth, and countless others, CHAI and government partners cannot let down their vigilance in addressing the disparity between ORS and zinc uptake.

Source of Data: KDHS, 2014





